Transforming care by integrating maternity and psychological support: a mixed-methods evaluation of a Maternal Mental Health Service | BMC Pregnancy and Childbirth

Design & procedure
The study used a mixed methods design. This service evaluation was approved by the West London NHS audit committee. We followed the UK Health Research Authority decision tool to determine that research ethics approval was not required, as the project entailed a retrospective, anonymised analysis of routinely collected service data. Demographic data was obtained from online electronic client Rio records.
Setting
The North-West London (NWL) Maternity Trauma and Loss Care (MTLC) service is a MMHS that covers the eight NWL boroughs, as seen in Fig. 1, and comprises of two ‘sub teams’; the West London and the Central and Northwest London MTLC Service. This study sample will focus on the West London MTLC service, which covers the boroughs of Ealing, Hounslow and Hammersmith & Fulham, hereby referred to as ‘MTLC’. West-London has an ethnically diverse population; Ealing’s population is nearly 30% Asian, Asian British or Asian Welsh and nearly 11% is Black, Black British, Black Welsh, Carribean or African. Similarly, Hounslow’s population is almost 37% Asian, Asian British or Asian Welsh, and 7.2% identifies as Black, Black British, Black Welsh, Carribean or African. A larger proportion of the population identify as White in Hammersmith & Fulham (63.2%), with a smaller representation of Asian (10.5%) and Black British, Black Carribean or African (12.3%) [35]
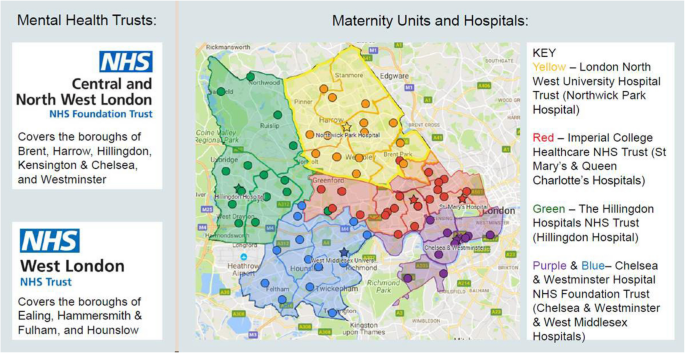
Map of MTLC coverage area
MTLC has an integrated team of specialist perinatal mental health midwives and psychological practitioners. The service accepts self-referrals and referrals from any other healthcare professionals, such as maternity, mental health teams and GPs.
The MTLC service is for individuals who have experienced a traumatic pregnancy or birth, perinatal loss (during pregnancy or within the first year of life), or have tokophobia (with or without previous experience of pregnancy). The eligibility criteria for referrals to MTLC include women and birthing people who are aged 18 or over and living within the West London geographical boundary. They must also either be currently pregnant or have been pregnant, given birth or had a perinatal loss within the last 12 months. If currently pregnant, clients need to be booked for their maternity care at a North-West London maternity hospital. Clients are seen in a variety of different clinic settings including maternity hospitals, children centres, GP surgeries and online via MS Teams.
Sample
The sample includes all clients who were referred to MTLC over the 12-month period from 1 st April 2022 to 31 st March 2023. The service received 254 referrals. Of the 254 referrals MTLC received, 14 referrals were re-referrals within the year i.e. referrals for clients that had already been referred within April 2022 and March 2023. Thus, 240 people were referred to MTLC in total. Of the 190 accepted referrals, 5 individuals were referred twice, accepted and offered an assessment. Therefore 185 clients were referred to MTLC and offered an assessment. Of these, 72 clients had paired, completed outcome measures and were included in the analysis.
Interventions
MTLC offers short-to-medium term interventions; up to 8 midwifery sessions and up to 24 psychological therapy sessions. MTLC aims to take an active role in preventing re-traumatisation and empowering women and birthing people throughout their maternity journeys.
One-to-one specialist midwifery care includes building trusting relationships with clients, offering evidence-based interventions to manage anxiety and fear, and help navigating the maternity system. The evidence-based support [36] also includes trauma-informed birth preparations where a collaborative approach aids the client and clinician to consider how to minimise the activation of previous trauma experiences, how to address labour-related challenges such as the client’s need for control and difficulties with disclosure. This is achieved through the MTLC midwives advocating for clients, as well as enabling clients and their birthing partners to advocate for themselves during pregnancy and childbirth. These factors are essential to create a positive birthing experience [37]. MTLC midwives also support clients in navigating complex maternity systems and advocating on their behalf during interactions with wider NHS services. Midwives working within MTLC are employed by the acute hospital trusts but hold honorary contracts with affiliated mental health trusts. Their roles are protected for exclusive delivery of MTLC care; thus, they do not undertake routine clinical duties within the acute maternity setting. This employment model facilitates the integration of psychologically informed midwifery practice within acute services.
The psychological interventions offered comprise NICE recommended and concordant interventions for perinatal trauma and loss. This includes Trauma-Focused Cognitive Behavioural Therapy (TFCBT), Eye Movement Desensitisation and Reprocessing (EMDR), Compassion Focused Therapy (CFT) and Acceptance and Commitment Therapy (ACT).
Trauma focused therapy is a specialised form of psychotherapy which helps individuals process and heal from traumatic experiences. The goal is to create a safe environment where clients can explore their feelings, understand the impact of trauma on their lives, and develop healthier coping mechanisms to help reduce symptoms such as anxiety, flashbacks, and emotional numbness. The benefits of trauma therapy are profound. It can enhance emotional resilience, improve relationships, and restore a sense of safety and control. Many individuals experience reduced PTSD symptoms, greater self-awareness, and an improved ability to handle stress [38].
All antenatal clients were offered an intervention of midwifery support, unless deemed not necessary, for example if they were receiving enhanced midwifery care from their maternity hospital or were more closely monitored by medical or obstetric teams. Where psychological needs were identified—either at initial assessment or during the antenatal period—clients were also offered psychological therapy alongside midwifery support. This integrated approach enabled coordinated care that addressed both the psychological and maternity-related needs of clients, promoting shared understanding and partnership between professionals and clients.
Guided by the NHS-endorsed TIC principles for perinatal mental health [39] —Compassion and Recognition, Communication and Collaboration, Consistency and Continuity, and Recognising Diversity and Facilitating Recovery, MTLC integrates these principles into all levels of its clinical delivery. MTLC places high value on transparent, two-way communication, enabling clients to make informed choices about their care.
The foundation of MTLC’s model is compassion that recognises the pervasive impact of trauma on the perinatal experience. Staff are trained to understand how trauma may shape a person’s engagement with care, even in the absence of disclosure. MTLC midwives offer one-to-one support, building therapeutic relationships through trust, emotional presence, and attuned listening.
Continuity of care is not routinely available in many maternity settings yet is a key protective factor against re-traumatisation. MTLC midwives, provide consistent, ongoing care from referral to postnatal discharge. This stability allows clients to avoid repeated disclosures of trauma and supports the development of trust over time.
The service actively engages with individuals whose needs are often underserved—those affected by perinatal loss, refugee and migrant communities, and people experiencing tokophobia. Culturally sensitive approaches and personalised care planning help address the varied ways in which trauma is experienced and expressed. Clinicians are encouraged to hold space for complex grief and identity formation during the perinatal period, especially for those with intersecting vulnerabilities such as past abuse, systemic racism, or socioeconomic disadvantage. This principle is also extended to the workforce, acknowledging that staff themselves may carry trauma histories, and offering reflective practice to mitigate vicarious trauma and compassion fatigue.
Demographic information
Demographic data collected included: ethnicity, borough of residence, pregnancy status, booking hospital and referrer.
Measurements
Clinical outcomes in routine evaluation (CORE-10)
The CORE-10 [40] is a 10-item patient-rated measure that considers both experienced symptoms of low mood, anxiety and functioning (ability to cope, availability of help) in the last week. While the validity in different ethnic groups has not been formally established, the measure is routinely used in the NHS for diverse populations. Responses are measured on a 5-point Likert scale: 0 (not at all) to 4 (most or all of the time). The score range is 0–40, with higher scores indicating higher distress. The CORE-10 was collected at assessment, before intervention, and at discharge from the MTLC service by the clinician carrying out the intervention (psychological therapist or midwife).
Post-traumatic stress disorder checklist for DSM-5 (PCL-5)
The PCL-5 [41] is a 20-item patient-rated measure that assesses the 20 DSM-5 symptoms of PTSD. The PCL-5 asks respondents how often they have been bothered by a symptom in the past month. Responses are measured on a 5-point Likert scale: 0 (not at all) to 4 (extremely). The score range is 0–80, with higher scores indicating higher distress. A PCL-5 score of 33 and above suggests a high likelihood of PTSD. The PCL-5 has a high demonstrated high internal reliability (α = 0.94) [42]. It was selected as an outcome measure due to its demonstrated validity in ethnically diverse groups [42]. The PCL-5 was collected at assessment, before intervention, and at discharge from the MTLC service by the clinician carrying out the intervention (psychological therapist or midwife).
Service user satisfaction survey
This survey was sent to all clients following treatment discharge. It is based on the NHS Friends and Family Test and was co-produced by experts by experience, who were part of mobilising the service. The survey asks clients to provide feedback on their experience of MTLC. Seven questions were quantitative in nature, with ratings determined on a five-point Likert-type scale by level of satisfaction ranging from unsatisfied to very satisfied, including a neutral option. Below these seven questions was the option to provide qualitative feedback on the topic the question asked about the service. For example, one question was ‘How much do you feel you were treated with kindness and respect by the staff in M-TLC?’ with the option to give a ranked response and an option to leave qualitative feedback. The survey further includes questions regarding treatment by staff, involvement in care and decisions, impacts of the support received from the service on emotional and mental wellbeing, and satisfaction with waiting times.
Analysis
Deprivation was assessed using the index of multiple deprivation (IMD) based on the postcode of the client [43]. Areas were assigned to deciles, where decile 1 represents the most deprived 10% of areas in England, and decile 10 represents the least deprived. For analysis, IMD deciles were grouped into three bands: among the 20% most deprived areas (deciles 1–2), among the 20–40% deprived areas (deciles 3–4), moderate deprivation (deciles 5–6), among the 20–40% least deprived areas (deciles 7–8), among the 20% least deprived areas (deciles 9–10).
Quantitative data including CORE-10 and PCL-5 scores, were extracted from the service electronic database RiO. Quantitative data that could not be extracted from the electronic databases were manually recorded by staff. Where required, data were cross referenced with individual client records. Confidentiality was respected and upheld during both the analysis and dissemination. Descriptive statistics for the referrals received were analysed reviewing the description of the clients’ demographic information, such as reason for referral, interventions offered and client ethnicity. Paired sample T-Tests were performed using IBM SPSS Statistics, version OS for Mac [44]. Qualitative feedback was gathered through completion of the Service User Satisfaction Survey. Recurrent themes throughout the surveys were identified and summarised.
link